Overview
Median Arcuate Ligament Syndrome (MALS) is an uncommon condition characterized by chronic, often debilitating abdominal pain caused by compression of the celiac artery and surrounding neural structures by the median arcuate ligament — a fibrous band of the diaphragm. Because the symptoms are frequently nonspecific and overlap with other gastrointestinal disorders, patients often undergo extensive evaluation before receiving a diagnosis.
As a complex general surgeon with extensive experience in advanced minimally invasive and robotic techniques, Dr. Jeffrey S Fronza has developed a focused practice in the diagnosis and surgical treatment of MALS. He has performed more robotic median arcuate ligament releases than any other surgeon in the state of Illinois.
Relevant Anatomy
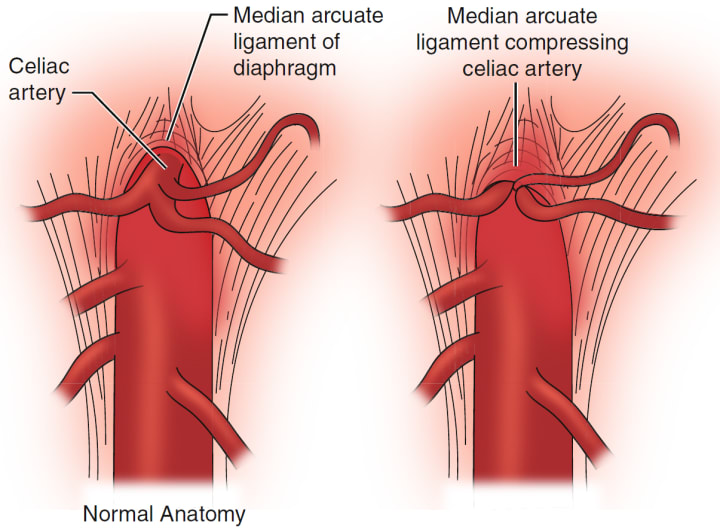
The celiac artery is one of the first major branches of the abdominal aorta. It supplies blood flow to the stomach, liver, spleen, and portions of the pancreas and duodenum. The median arcuate ligament is a fibrous arch formed by the right and left crura of the diaphragm that passes over the aorta.
In some individuals, this ligament lies lower than usual and compresses:
- The celiac artery, potentially altering blood flow dynamics
- The celiac plexus, a dense network of autonomic nerves surrounding the artery
Both vascular and neurogenic mechanisms are believed to contribute to symptoms.
Proposed Pathophysiology
The exact cause of symptoms in MALS remains an area of ongoing research. Current understanding suggests a combination of:
-
Vascular Compression
Dynamic compression of the celiac artery — often worse during expiration — may reduce blood flow to the foregut organs, particularly during periods of increased demand such as eating.
-
Neurogenic Irritation
Compression and irritation of the celiac plexus may result in chronic neuropathic pain independent of measurable blood flow restriction.
Most experts believe that symptoms arise from a combination of these mechanisms rather than purely arterial narrowing alone.
Common Symptoms
Patients may experience:
- Postprandial (after eating) epigastric pain
- Unintentional weight loss
- Early satiety
- Nausea
- Exercise-induced abdominal discomfort
Because imaging findings alone do not confirm symptomatic MALS, careful clinical evaluation is essential.
Diagnostic Evaluation
Evaluation typically includes:
- CT angiography (CTA) or MR angiography (MRA)
- Duplex ultrasound demonstrating elevated celiac artery velocities
- Assessment for dynamic respiratory variation
- Careful exclusion of other gastrointestinal causes of pain
Successful treatment depends on appropriate patient selection.
Surgical Treatment: Robotic Median Arcuate Ligament Release
For appropriately selected patients, surgical release of the median arcuate ligament offers the best opportunity for symptom improvement.
Dr. Jeffrey S Fronza performs this procedure using a robotic minimally invasive approach, which provides:
- High-definition three-dimensional visualization
- Precise dissection around critical vascular structures
- Enhanced dexterity for safe release of the ligament and surrounding fibrotic tissue
Procedure Overview
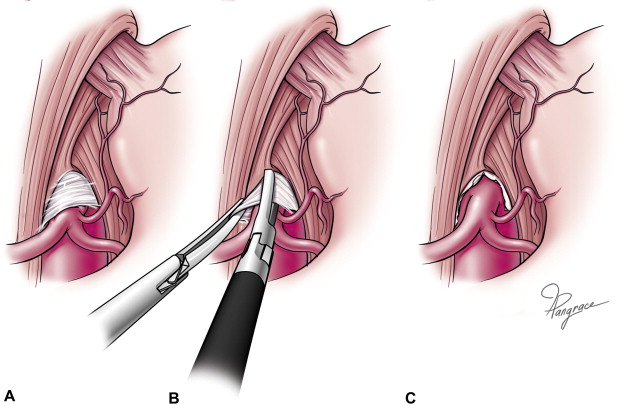
The operation involves:
- Careful exposure of the celiac axis
- Complete division of the median arcuate ligament
- Thorough neurolysis of the celiac plexus
- Confirmation of decompression of the celiac artery
Recovery
Because the operation is performed robotically:
- Patients are discharged the day after surgery
- Postoperative pain is typically manageable
- Return to normal activity occurs over several weeks
Symptom improvement may be gradual as neural inflammation resolves.
A Specialized, Thoughtful Approach
MALS is a nuanced diagnosis that requires thoughtful evaluation and technical expertise. Not every patient with radiographic compression benefits from surgery, and careful clinical judgment is essential.
Dr. Fronza’s approach emphasizes:
- Rigorous patient selection
- Detailed preoperative evaluation
- Technical precision in robotic decompression
- Longitudinal postoperative follow-up
If you have been diagnosed with MALS or are seeking a second opinion regarding chronic unexplained abdominal pain, consultation may help clarify whether surgical treatment is appropriate for you.